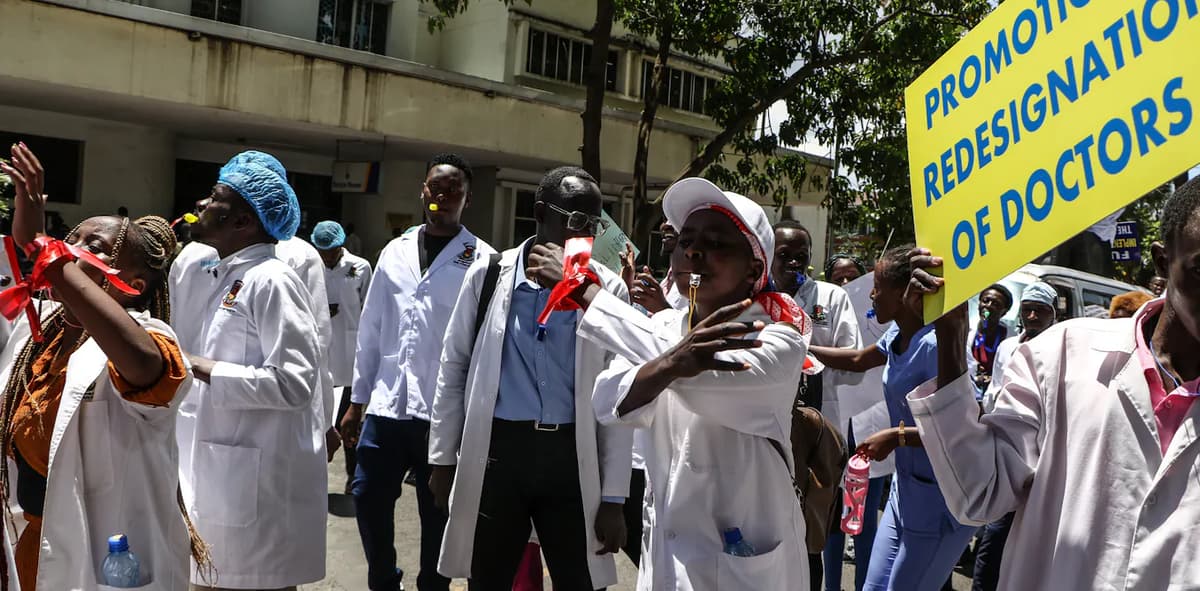
Africa Is Losing Health Workers when It Can Least Afford to – a Pattern Rooted in Colonial History
Why It Matters
The exodus weakens African health systems, jeopardizing universal health coverage, while high‑income countries save billions on training costs, deepening global inequity.
Key Takeaways
- •Africa may lose 5‑6 million health workers by 2030
- •Only four African nations meet WHO’s 4.45 per 1,000 benchmark
- •High‑income countries saved billions by recruiting African clinicians
- •Colonial power structures shape migration beyond simple push‑pull factors
Pulse Analysis
The projected deficit of 5‑6 million health workers in Africa is more than a staffing issue; it threatens the continent’s ability to meet basic health needs and achieve universal health coverage. While the World Health Organization flags a global shortfall of 11 million, Africa’s disproportionate share stems from chronic under‑investment, low salaries, and fragile health infrastructure. These conditions create a fertile ground for migration, especially as high‑income countries grapple with their own workforce gaps and turn to overseas talent to fill vacant positions.
Beyond the conventional push‑pull narrative, the migration stream mirrors a colonial legacy that still structures global health labor markets. Wealthier nations often under‑invest in domestic training, then harvest skilled professionals from former colonies, effectively externalising the cost of education. Studies estimate that sub‑Saharan African states lose billions of dollars in training investments, while recipient countries reap savings and bolster their health systems. Simultaneously, the dominance of Western medical curricula devalues African qualifications, compelling clinicians to seek validation abroad and reinforcing a hierarchy of knowledge that privileges the Global North.
Addressing this imbalance requires systemic reforms rather than individual incentives. Ethical recruitment codes must be enforced, and high‑income countries should fund capacity‑building initiatives or reparative investments in African health education. Circular migration schemes and bilateral training agreements can enable skill exchange without permanent brain drain. Crucially, recognizing and integrating Southern medical expertise into global standards will dismantle the lingering colonial bias, fostering a more equitable and resilient global health workforce.
Africa is losing health workers when it can least afford to – a pattern rooted in colonial history
Comments
Want to join the conversation?
Loading comments...