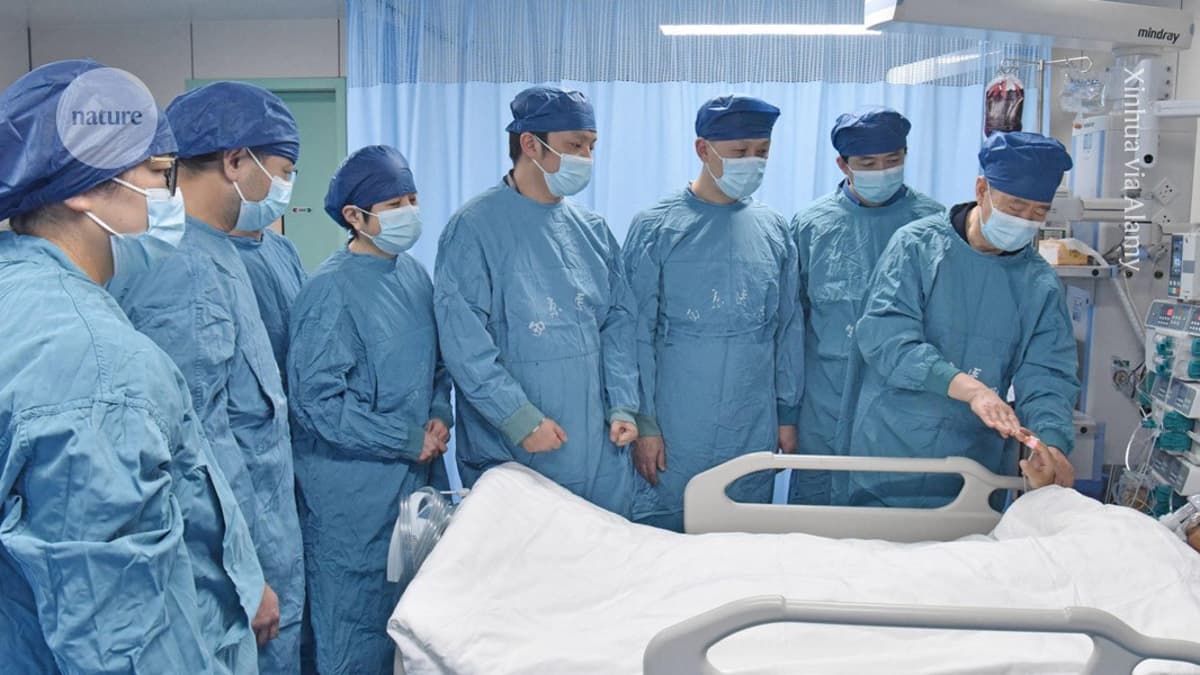
Genetically Modified Pig Liver Keeps Man Alive Until Human Organ Transplant
•March 6, 2026
0
Why It Matters
The success demonstrates that gene‑edited pig organs can safely sustain human physiology, offering a potential lifeline for patients on transplant waiting lists and easing the chronic organ shortage.
Key Takeaways
- •First living patient linked to gene‑edited pig liver externally.
- •Six genetic edits reduced rejection risk during extracorporeal perfusion.
- •Procedure bought time until human liver transplant, patient now recovering.
- •Xenotransplantation may become bridge therapy for organ‑waitlist patients.
- •Clinical data on immunosuppression and duration still needed.
Pulse Analysis
Organ scarcity remains a critical bottleneck in modern healthcare, with thousands dying each year while awaiting donor livers. Xenotransplantation—using animal organs modified to resemble human tissue—has progressed from experimental trials to clinical applications over the past decade. Early successes with pig hearts and kidneys have paved the way for more complex organs, and regulatory bodies in the United States and China are actively reviewing protocols to accelerate safe adoption. This broader context underscores why a living‑patient bridge using a pig liver is a watershed moment.
The Chinese team at Xijing Hospital employed a pig liver engineered with three deactivated pig genes and three human genes that produce protective proteins, dramatically reducing immune activation. By connecting the organ to a perfusion circuit through a leg vein, clinicians redirected the patient’s blood, allowing the pig liver to filter toxins and support metabolic functions for several days. No acute rejection signs emerged, and the patient’s native liver showed functional improvement, enabling a timely transition to a human donor organ. Such extracorporeal perfusion differs from full implantation, offering a reversible, controllable platform to assess compatibility and fine‑tune immunosuppressive regimens.
Looking ahead, this breakthrough could reshape transplant economics and logistics. Hospitals may adopt pig‑organ bridge systems as standard interim care, reducing intensive‑care costs and improving survival odds. However, long‑term data on immunosuppression intensity, duration limits, and potential zoonotic risks are essential before widespread rollout. Investors and biotech firms are likely to accelerate R&D in gene‑editing tools and perfusion technologies, while policymakers will need to balance innovation with rigorous safety oversight. If these challenges are met, xenogeneic bridge therapies could become a cornerstone of organ‑failure treatment, alleviating pressure on donor registries worldwide.
Genetically modified pig liver keeps man alive until human organ transplant
0
Comments
Want to join the conversation?
Loading comments...