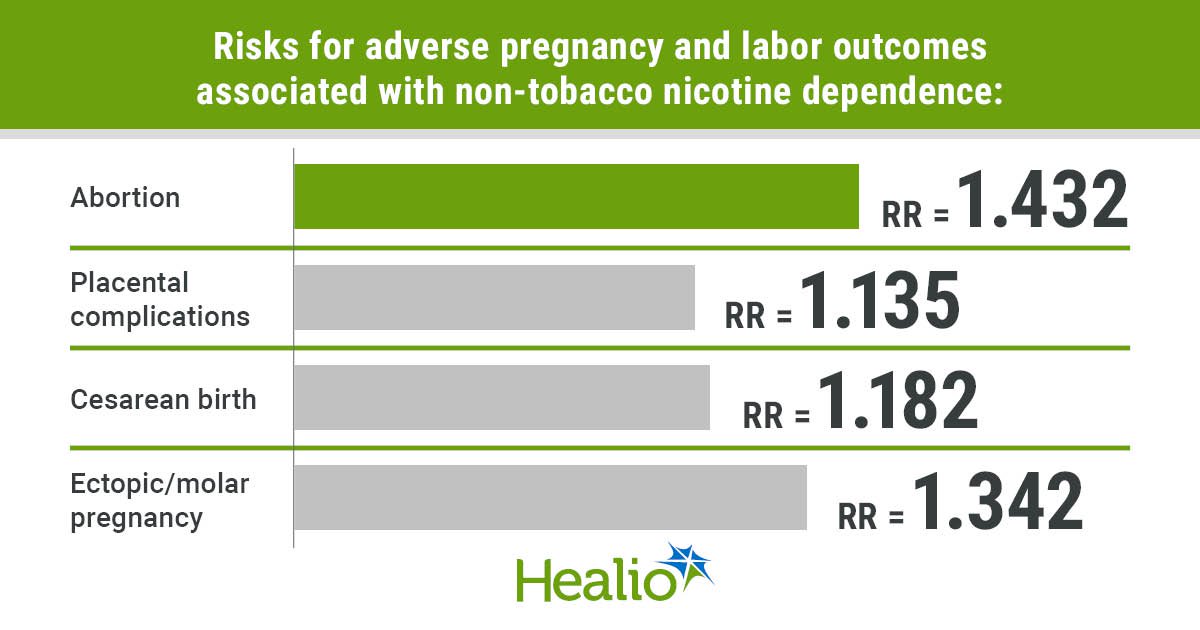
Non-Tobacco Nicotine Products Tied to Pregnancy, Labor Complications
Why It Matters
The findings broaden the scope of prenatal risk assessment, compelling obstetric providers to screen for all nicotine products, not just cigarettes, and prompting public‑health campaigns to address misconceptions about vaping safety.
Key Takeaways
- •Non‑tobacco nicotine use raises risk of preterm labor by 72%
- •Vaping linked to 2.5‑fold increase in maternal death during pregnancy
- •Opioid abuse risk spikes over 15‑fold among nicotine‑using pregnant patients
- •Study of 77,549 women shows higher cesarean and emergency‑room visits
- •Researchers urge broader nicotine screening beyond traditional cigarettes in prenatal care
Pulse Analysis
The rapid adoption of vaping and nicotine pouches among women of reproductive age has outpaced the scientific literature, creating a perception gap where many assume these products are harmless alternatives to cigarettes. While traditional tobacco smoking has long been linked to poor obstetric outcomes, the nicotine itself—delivered via aerosols, gums, or lozenges—exerts vasoconstrictive and neuroendocrine effects that can compromise placental perfusion and fetal development. This study leverages the expansive TriNetX database to provide the first large‑scale, propensity‑matched analysis of non‑tobacco nicotine exposure, offering a data‑driven counterpoint to the prevailing safety narrative.
The analysis revealed a striking elevation in a spectrum of complications. Preterm labor risk rose by 72%, and the odds of cesarean delivery increased by 18%, underscoring how nicotine’s hemodynamic impact translates into tangible delivery challenges. More alarming were the severe outcomes: maternal mortality more than doubled, and myocardial infarction risk more than doubled as well. The association with opioid abuse—over a 15‑fold increase—suggests that nicotine use may serve as a marker for broader high‑risk behaviors, amplifying the need for integrated substance‑use screening in prenatal visits. These relative risks, derived from a cohort of nearly 80,000 patients, provide a robust epidemiological signal that cannot be dismissed as anecdotal.
Clinically, the study mandates a shift in counseling protocols. Obstetricians must explicitly inquire about all nicotine delivery systems, not merely combustible tobacco, and incorporate tailored cessation resources that address the unique behavioral patterns of vaping users. Health systems should update electronic health record prompts to capture non‑tobacco nicotine use, enabling early intervention. Policymakers may also consider extending warning labels and public‑health campaigns to encompass e‑cigarettes and nicotine pouches. Future research should dissect product‑specific risks and explore longitudinal outcomes, but the current evidence already justifies a more aggressive, comprehensive approach to nicotine screening in pregnancy.
Non-tobacco nicotine products tied to pregnancy, labor complications
Comments
Want to join the conversation?
Loading comments...