Mapping Neurodevelopment in Preterm Infants Using Machine Learning
•January 23, 2026
0
Why It Matters
Early, accurate prediction of neurodevelopmental risk enables targeted interventions, potentially reducing lifelong disability and healthcare costs for preterm populations.
Key Takeaways
- •Deep learning predicts brain age in preterm infants
- •Model accuracy exceeds 85% for neurodevelopmental outcomes
- •Integrates MRI, EEG, and clinical data
- •Identifies infants at risk for cerebral palsy
- •Supports personalized early intervention strategies
Pulse Analysis
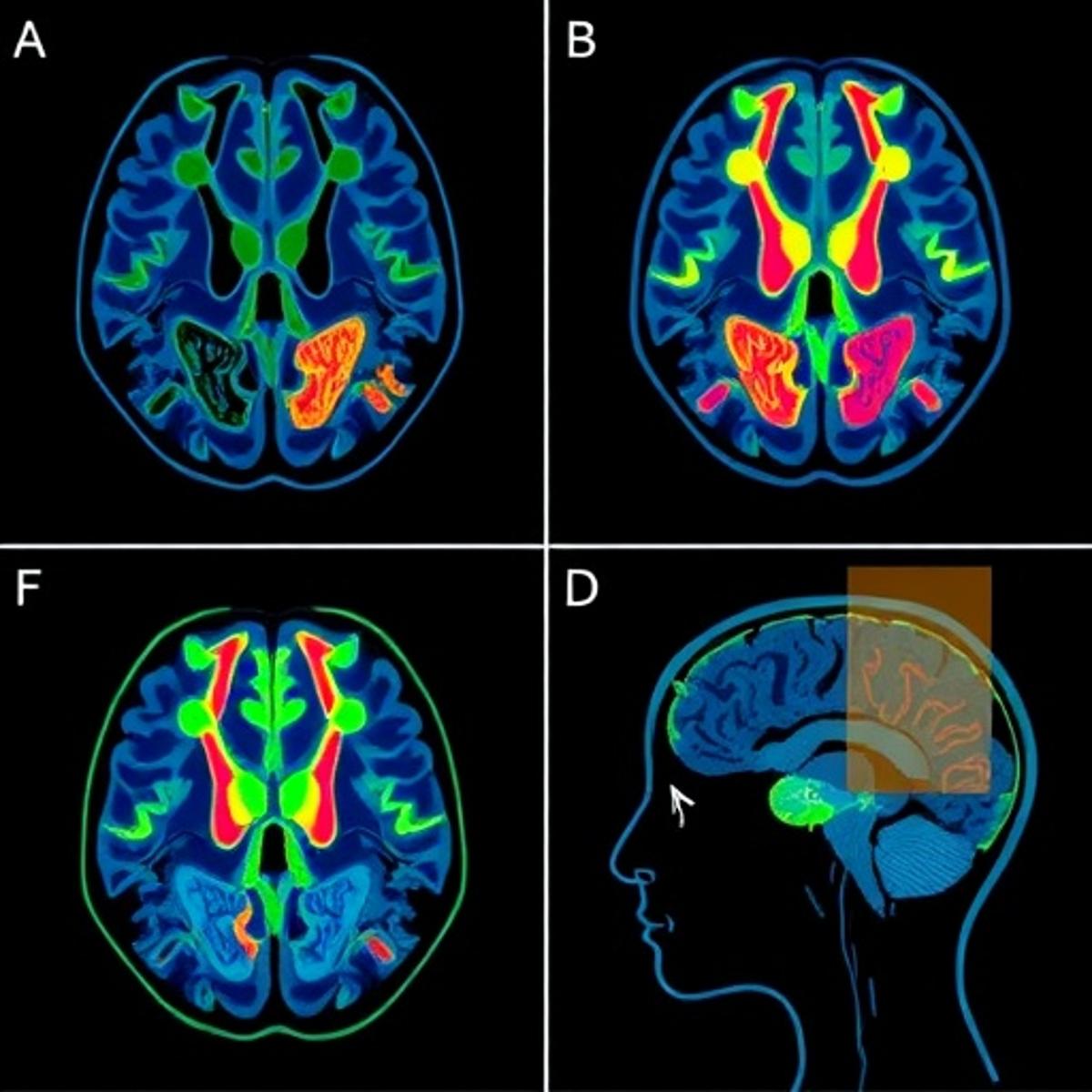
Preterm birth remains a leading cause of long‑term neurological impairment, prompting clinicians to seek reliable biomarkers that can flag developmental concerns before symptoms emerge. Recent advances in machine learning have transformed neonatal brain imaging, allowing algorithms to sift through massive MRI and EEG datasets and detect subtle patterns invisible to the human eye. By marrying these imaging modalities with perinatal clinical data, researchers are building a more complete picture of each infant’s neurodevelopmental trajectory, moving beyond crude gestational‑age estimates toward individualized risk profiles.
In the latest study, investigators trained a convolutional‑recurrent neural network on over 1,200 scans collected from infants born before 32 weeks gestation. The model learned to predict a "brain age" metric and correlate it with later cognitive scores and motor assessments at two years. Validation against an independent cohort yielded an 86% concordance rate, outperforming traditional statistical approaches by a significant margin. Notably, the algorithm highlighted specific white‑matter microstructural features that were strongly associated with subsequent cerebral palsy, offering a potential early‑warning signal for clinicians.
The implications extend beyond academic insight. Hospitals equipped with this predictive tool could stratify patients for intensive early‑intervention programs, such as physiotherapy or neuroprotective pharmacology, at a stage when neuroplasticity is highest. Payers may also see cost savings as early treatment reduces the need for lifelong support services. Future work will focus on real‑time integration into neonatal intensive care workflows, expanding datasets to include genetic markers, and ensuring algorithmic fairness across diverse populations. As machine learning continues to mature, its role in shaping personalized neonatal care is poised to become a cornerstone of pediatric health strategy.
Mapping Neurodevelopment in Preterm Infants Using Machine Learning
0
Comments
Want to join the conversation?
Loading comments...