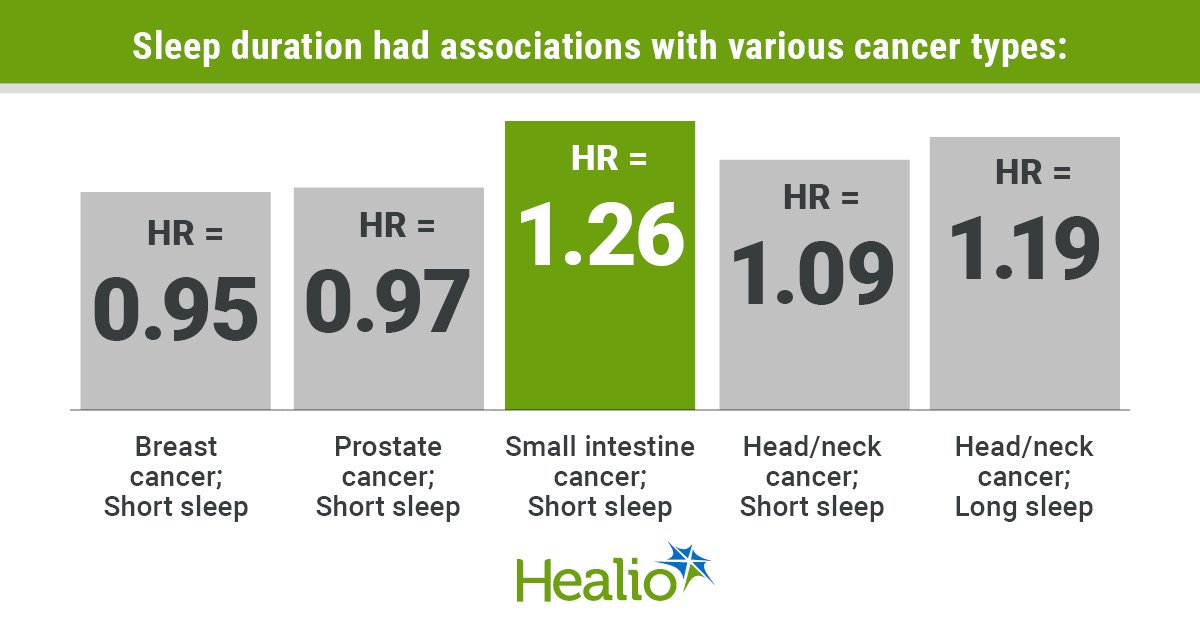
Sleep Duration Has ‘Complex’ Association with Cancer
Why It Matters
Understanding how sleep patterns influence cancer risk can refine public‑health recommendations and guide clinicians in personalized counseling. It also creates a market for objective sleep monitoring tools to support preventive oncology.
Key Takeaways
- •Short sleep (<7h) modestly lowers overall cancer risk (HR 0.98).
- •Short sleep raises risk for small‑intestine, head‑neck cancers, AML.
- •Restless sleep increases hepatocellular carcinoma risk, lowers breast and rectal risk.
- •Long sleep shows non‑significant risk elevation; only 5% reported long sleep.
Pulse Analysis
Sleep research has long linked insufficient rest to cardiovascular disease and mortality, but its relationship with cancer remains murky. Recent epidemiological work leverages large, diverse cohorts to tease apart how both quantity and quality of sleep intersect with oncogenesis. By aggregating data from nearly a million participants, investigators can control for confounders such as age, sex, and lifestyle, offering a more granular view than earlier single‑study analyses that often produced contradictory conclusions.
The meta‑analysis reveals a paradox: while sub‑7‑hour sleepers exhibit a modest dip in overall cancer incidence, they face heightened odds for rarer but aggressive cancers like small‑intestine malignancies, head‑and‑neck tumors, and acute myeloid leukemia. Conversely, short sleep appears protective for hormone‑driven cancers such as breast and lung, suggesting that sleep‑related hormonal modulation may play a role. Restless or fragmented sleep further complicates the picture, boosting liver cancer risk while slightly reducing breast and rectal cancer rates. These nuanced patterns underscore that a one‑size‑fits‑all sleep prescription may be overly simplistic for cancer prevention.
Future research will likely pivot toward objective sleep tracking via wearables and nearables, reducing reliance on self‑reporting and capturing circadian timing, sleep efficiency, and variability. Integrating such granular data with genomic and exposomic profiles could enable risk stratification tools for clinicians. Policymakers may also reconsider current sleep guidelines, emphasizing not just duration but consistency and quality, to align public‑health messaging with emerging evidence that sleep’s impact on cancer is both protective and hazardous, depending on the disease context.
Sleep duration has ‘complex’ association with cancer
Comments
Want to join the conversation?
Loading comments...