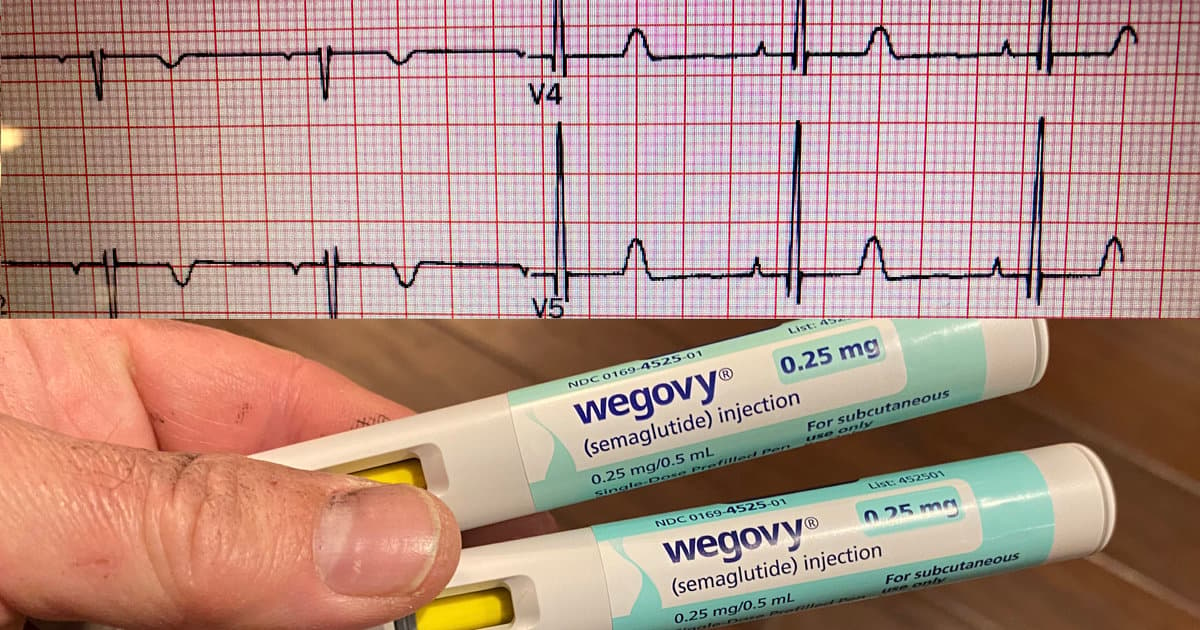
Multiple GLP-1 Drugs Linked to Lower AFib Risk
Why It Matters
GLP‑1 therapies could become a dual‑purpose tool for diabetes, obesity, and AFib prevention, reshaping cardiovascular risk management. The findings may prompt clinicians to consider rhythm benefits when selecting GLP‑1 agents, influencing prescribing patterns and drug development priorities.
Key Takeaways
- •GLP‑1 agonists cut atrial fibrillation incidence in >13k patients.
- •Risk reduction persists regardless of weight loss magnitude.
- •Semaglutide shows strongest AFib protection among GLP‑1 drugs.
- •Study matched 13,034 treated vs 385,000 controls.
- •Improved survival observed alongside lower AFib rates.
Pulse Analysis
Atrial fibrillation remains the most common sustained arrhythmia, affecting millions worldwide and driving hospitalizations, stroke, and mortality. While weight loss and glycemic control have long been recognized as modifiable risk factors, the emergence of GLP‑1 receptor agonists (GLP‑1 RAs) has introduced a novel therapeutic class that may influence cardiac electrophysiology directly. By binding to GLP‑1 receptors in myocardial tissue, these agents can modulate autonomic tone, reduce inflammation, and improve endothelial function—mechanisms that plausibly curb the substrate for AFib beyond mere metabolic effects.
The recent single‑center, retrospective cohort presented at Heart Rhythm 2026 leveraged electronic health records to compare 13,034 GLP‑1‑RA initiators with a propensity‑score‑matched control group of more than 385,000 patients without prior AFib. The analysis revealed a statistically significant drop in new‑onset AFib, independent of the degree of weight change, suggesting intrinsic anti‑arrhythmic properties. Notably, semaglutide, the most potent GLP‑1 RA in terms of glucose lowering and weight reduction, exhibited the greatest risk attenuation, hinting at dose‑response or pharmacokinetic nuances that merit deeper investigation.
For clinicians, these findings broaden the value proposition of GLP‑1 RAs, positioning them as potential agents for primary AFib prevention in high‑risk populations such as diabetics and obese patients. Payers may reassess formulary decisions as cardiovascular outcome data accumulate, while pharmaceutical developers could explore combination trials with established anti‑arrhythmic drugs. Future prospective studies are essential to confirm causality, delineate mechanisms, and define optimal patient selection, but the current evidence already signals a shift toward integrated metabolic‑cardiac therapeutics.
Multiple GLP-1 drugs linked to lower AFib risk
Comments
Want to join the conversation?
Loading comments...