
New Apple, LinkedIn Leaders Prove Next CEO Should Already Be Working for You
Apple and LinkedIn have each appointed long‑time insiders—John Ternus and Daniel Shapero—as their next CEOs, underscoring a deliberate shift toward internal succession. Both leaders highlighted AI‑driven transformation and a commitment to maintaining strong workplace culture. The announcements were framed as signals of stability, aiming to boost employee confidence and retention. Leadership‑development experts note that promoting from within can reduce perceived volatility and reinforce long‑term career pathways.

How AI Is Changing the Face of Benefits Advising
Artificial intelligence is transforming employee benefits advising from a reactive, research‑heavy model to an anticipatory, data‑driven service. WTW’s AI assistant, Expert, automates tasks such as drafting job descriptions and benchmarking, allowing consultants to focus on organizational design. Businessolver’s Sofia adds...

Why Focus Time Should Be Treated as an Employee Benefit
The article argues that uninterrupted focus time should be treated as a core employee benefit rather than an optional perk. Research of 140,000 workers shows most employees only get two to three hours of deep work each day, with the...

Rising Medical Costs, Inflation Amplify Employee Financial Stress
Prudential’s 2026 Benefits & Beyond study finds rising medical costs are deepening employee financial stress, with 70% of U.S. workers reporting some level of strain and 28% describing it as significant. Employer‑sponsored family health premiums averaged $26,993 in 2025, a...

Trump Administration Wants Fed Job Applicants to Disclose Political Affiliations
The Office of Personnel Management’s Merit Hiring Plan now adds optional political‑essay prompts to federal job applications, appearing on roughly 33,000 postings—about a quarter of competitive listings. While the essays are currently optional, the Trump administration has hinted they could...

6 Tips for Reviewing Vendor Contract Terms
Performance guarantees such as "zero increase" pricing are now common in health‑benefit vendor renewals, but their real value hinges on precise contract language. Brokers must verify what costs are covered, how baselines are set, and which exclusions apply. Clear measurement...

How AI Can Enhance Benefit Leader, Broker Relationships
Gyde, a brokerage‑focused AI firm, launched its GydeOS platform and Gia assistant to shift benefit brokers from pure administrative tasks to proactive healthcare navigation. The tools automate calendar management, product recommendations, outreach, and renewal handling, freeing brokers to engage in...

Turning Mental Health Parity Into Progress Now a Business Imperative
Voya’s State of Employee Benefits 2026 report finds mental health at the core of employee well‑being, with 91% of employers saying it positively impacts overall health. One‑in‑five U.S. adults experience mental illness annually, and gaps in provider availability, cost and...

How to Build a Nationwide Hiring Process for Remote Roles
Remote work has turned talent acquisition into a national contest, prompting HR leaders to design hiring processes that work across state lines. The article outlines how organizations can align hiring strategy with business goals, standardize role definitions, and build a...
Costco, Sesame, IVI RMA Partner on Fertility Care Where Employers Often Fall Short
Costco, self‑pay marketplace Sesame, and global clinic IVI RMA have teamed up to offer a fertility‑care membership that bundles virtual expert guidance, diagnostic support and clinic referrals. The service costs $119 per month for the general public and $99 for Costco...

Why Payers Must Lead the Charge for Better Employer-Sponsored Healthcare
Zelis’ State of the Healthcare Financial Experience report shows employers are moving beyond pure cost control, treating benefits as a strategic lever for talent attraction, productivity, and retention. Sixty percent of benefits leaders now rate employee satisfaction as “very important,”...

Just Half of U.S. Workers Making Living Wage as Costs Rise
A Dayforce study finds only 51% of full‑time U.S. workers earn a living wage, a 5‑point decline since 2021. Women, Black and Latino employees fall far behind, with 44%, 31% and 33% respectively meeting the benchmark. Regional gaps persist, Texas...

Is Personal Security the New Must-Have Benefit?
Employers are adding 24/7 personal‑security platforms such as Our Bond as voluntary benefits to address a three‑decade high in U.S. safety fears. The mobile app connects employees to live agents, shares location, dispatches emergency assistance and can add services like bodyguards...

Why 'Insurance for Living' Can't Wait
The World Life Insurance Report 2026 reveals a stark mismatch between younger workers’ expectations and what insurers deliver in group life coverage. Only 19% of carriers provide portable policies, while 44% of under‑40 employees want coverage that follows them across jobs....

How Valvoline Is Driving Mental Health Support with Ronald McDonald House
Valvoline Inc. pledged $750,000 over three years to fund behavioral‑health services at Ronald McDonald House, directing $25,000 each year to ten chapters for counseling, therapy and crisis care. The partnership also launches a store‑wide donation drive through May 31, allowing customers to add...

A Shift in Retirement: Why More Companies Back Guaranteed Income
Employers are increasingly redesigning 401(k) plans to include guaranteed lifetime income options, reflecting a broader shift away from lump‑sum withdrawals. MetLife’s 2026 Lifetime Income Poll shows 90 % of defined‑contribution sponsors view income generation as the plan’s core purpose, with 59 %...

Benefit Brokers Consider Efficacy of Medical Cannabis
Benefit brokers are evaluating employer reimbursement of medical cannabis as a new health‑benefit option. Platforms such as EM2P2 already provide $100‑$175 per month stipends to cover physician‑authorized cannabis purchases. The recent federal downgrade of cannabis to Schedule III and HHS’s wellness...

Why Genetic Screening Should Be a Family Benefit
Employers are urged to add population‑based pediatric genetic screening to their benefits portfolios as a preventive health measure. Advances in sequencing technology and updated pediatric guidelines make early detection feasible, while the hidden costs of undiagnosed childhood conditions—missed workdays, stress,...

Language Learning Benefits Are a Must for Gen Z Talent
Language learning is evolving from a hobby into a strategic career mobility tool for Gen Z. Preply’s data shows 90% of Gen Z have collaborated with colleagues who speak a different first language, and 26% prioritize career advancement as their main motivation...

The 'Broken Handoff' Leaving Retirees Lost on Medicare Choices
Retirees exiting employer‑sponsored health plans often receive only a COBRA notice, leaving a "broken handoff" to Medicare advisers. Without coordinated guidance, many miss the initial enrollment window, incurring lifelong premium penalties and suboptimal plan choices. The issue affects roughly 10,000...

An Interactive Center Lets Leaders Take Accommodation Tools for a Test Drive
The Standard insurance company opened an interactive accommodation center in Portland, Oregon on June 1, giving employer customers hands‑on experience with tools that help employees stay or return to work. The space, part of the Workplace Possibilities program, showcases equipment for...

6 Tips for Creating a Competitive Compensation Model
Businesses that ignore total‑reward strategies risk higher turnover and recruiting expenses. The article outlines six practical steps—starting with market‑based salary benchmarking, conducting regular pay‑equity audits, expanding compensation beyond base salary, designing flexible pay bands, leveraging external expertise, and maintaining transparency—to...

The Power of Digitizing the Paycheck
The article argues that the traditional bi‑weekly payroll cycle is outdated in a digital economy, creating cash‑flow gaps for workers. It highlights research showing that granting earned‑wage access (EWA) can raise effective monthly income by over 11%, roughly $334, without...

Employers Are Investing in Virtual Care to Close Healthcare Gaps
Employers are rapidly adopting virtual‑first primary care, with 44% planning to add such services within the next year, according to Brown & Brown. The shift moves telehealth from a pandemic‑era stopgap to a core benefit expectation, enabling coordinated episodes of...

Healthy Workers Are Ditching Company Insurance to Save $1,000 a Month
Rising health‑care premiums are prompting healthy, young workers to abandon employer‑sponsored insurance in favor of cheaper alternatives. A Buffalo nurse and her family saved $970 per month by joining a medical‑cost‑sharing cooperative and enrolling their children in a state child‑health...
How Disintermediation Is Being Managed in Rx Models
Employers are moving away from traditional, single‑vendor pharmacy benefit managers, with transparent PBM adoption climbing to 31% in 2025 from 12% in 2024. This disintermediation creates multi‑vendor configurations that split claims, rebates, specialty management, and clinical navigation across separate partners....

Companies that Invest in Women Outperform Competition
New research from the Milken Institute’s Employer Action Exchange shows that companies offering integrated benefits, policies, and supportive cultures for women see markedly higher growth. The study, covering 11 years of data, links such programs to a 12‑percentage‑point outperformance versus...

For Disabled Employees, Financial Security Depends on Benefits and Guidance
Voya reports that households with an adult with a disability need 28% more income than average. One in five disabled employees face discrimination when seeking financial‑planning support. The article urges employers to align workplace benefits with public programs such as...

Employees Are Ditching Benefits for Their Own Health Apps
Castlight Health’s 2026 Employer Health Benefits Experience Survey shows most U.S. employees are sidestepping employer‑provided wellness programs in favor of personal digital health tools. Only about one‑third understand or regularly use their benefits, while 46% pay out‑of‑pocket for apps they...

How to Raise Broker Comfort with ICHRAs
Individual Coverage Health Reimbursement Arrangements (ICHRA) have surged, climbing more than 1,000% over the past five years and tripling in enrollment between 2024 and 2025. Employers are turning to ICHRA to lock in predictable healthcare spending, with Benefitbay reporting average...

Building a Culture that Thrives Through Change
Dayne Williams, CEO of Quantum Health, draws on his football quarterback experience to outline three leadership principles for navigating relentless change. He emphasizes building trust through authentic action, over‑communicating the purpose behind change, and fostering resilience via collective accountability. The...

Employers See 507% ROI From Behavioral Healthcare, New Study Shows
A new Integrated Benefits Institute study of ComPsych data shows employers can expect a 507% return on investment from behavioral health programs, translating to $6.07 saved for every dollar spent. Clinical outcomes were strong, with 63% of participants improving in...

LTC Coverage Emerging as a Necessary Consideration
Long‑term care (LTC) insurance is gaining traction as a core component of employee benefits, driven by the rise of hybrid life‑LTC policies that preserve the death benefit while providing care coverage. Traditional standalone LTC plans have become scarce and expensive,...

Why Gen Z's AI Skillset Isn't Translating to the Workplace
A recent Arkansas State University survey finds 26% of employers say entry‑level hires fall short on AI skills, and 18% have rejected Gen Z candidates for lacking AI expertise. While Gen Z is comfortable with tools like ChatGPT, Claude and Gemini, their...

A Comprehensive Checklist to Boost Caregiving Support for Employees
U.S. caregivers now represent roughly 44.6 million people, delivering unpaid labor valued at $873.5 billion annually. Employee Benefit News reports that half of caregiving workers anticipate heavier duties, and the strain is already affecting productivity. The National Employer Benefits and Health Group...
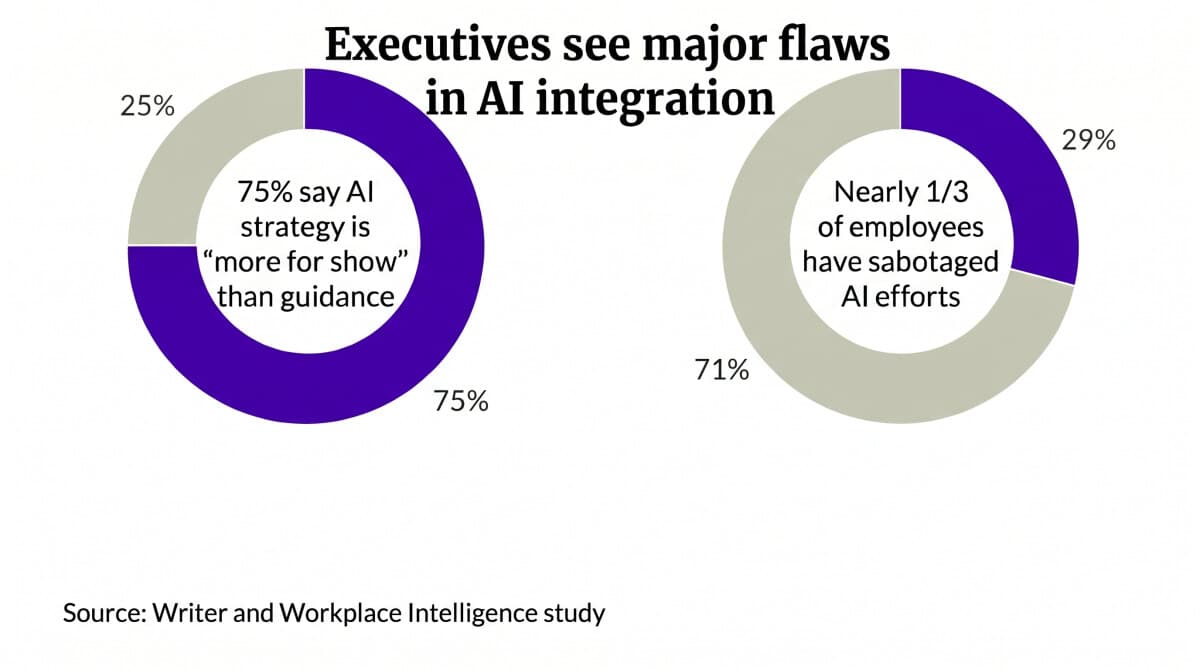
'Just for Show': Superficial AI Strategies Are Ruining Adoption
Executives are touting AI‑centric strategies, yet employee buy‑in remains shallow. A Betterworks survey shows 59% of leaders claim a clear AI vision, but only 8% of workers agree. Research by Writer and Workplace Intelligence finds AI super‑users are five times...

How to Show Appreciation for Retiring Employees
Organizations are confronting a surge in retirements and must move beyond paperwork to intentional recognition. Thoughtful retirement appreciation safeguards institutional knowledge, reinforces culture, and signals that long‑term contributions matter. Companies are urged to align recognition with core values, personalize the...

Financial Firms Expand Pooled Retirement Plans for Small Employers
Finance firms are expanding pooled employer plans (PEPs) to give small businesses and nonprofits a streamlined, 401(k)-style retirement option. Equitable introduced a new 403(b) PEP tailored for nonprofit employers, while KeyBank now manages over $250 million in PEP assets for 17...
How Employers End up Paying for Weight Gain
Employers are rapidly adding GLP‑1 weight‑loss drugs to health plans, but more than half of participants abandon therapy within a year, eroding the expected return on investment. While some firms pair prescriptions with nutrition coaching and behavior‑change programs, only about...

A Concierge Benefit Tackles Personal To-Do Lists, Boosts Productivity
Overalls, a concierge benefit platform launched in 2021, consolidates personal‑assistance services—from home repairs to medical navigation—into a single employee offering. Research of 1,350 workers shows non‑work hassles consume up to 17% of work time, while Overalls returns an average of...

Pets at Work? How Benefit Teams Can Prep to Accommodate Service Animals
Employers are increasingly encountering requests to bring service or emotional‑support animals to the office, a practice recognized as a reasonable accommodation under the ADA. Legal experts note a post‑pandemic surge in such inquiries, spanning dogs, miniature horses and even less...

Why Advisers Must Move From 'Retailers' To 'Guardians'
U.S. commercial healthcare consumes about $1.3 trillion annually, with roughly $325 billion—equivalent to a $4,000 per‑employee leak—attributed to administrative waste and opaque PBM pricing. Traditional benefits brokers earn commissions tied to premium volume, creating a direct conflict between adviser income and client...

Why More U.S. Workers Are Hitting the Panic Button
Workplace safety is under heightened scrutiny as solo‑worker incidents surge, with nearly 70% of U.S. companies reporting an event in the last three years and a 9% rise in homicides—the highest in a decade. Several states, including New York and Washington,...

Tom Brady's New Play: Making GLP-1s Affordable for Healthcare Workers
Tom Brady, co‑owner of eMed, is launching an employer‑subsidized GLP‑1 program aimed at U.S. healthcare workers. Employers pay a fixed $25 per employee each month, while employees cover $99 for medication and 24/7 clinical support. eMed reports participants lose an...

Why It Pays to Play the Long Game on Advanced Primary Care
Employer‑sponsored insurance plans are seeing urgent‑care spending jump more than 50% between 2018 and 2022, signaling a shift toward fragmented, quick‑care services. In response, many employers are adopting advanced primary care models that emphasize prevention, chronic‑disease management, and sustained patient‑provider...

How Life Expectancy Expectations Shape Retirement Saving Habits
A new TIAA Institute report finds that workers who expect longer retirements save significantly more, while only one‑third of Americans correctly estimate life expectancy at age 65. Those who anticipate a 30‑year or longer retirement are far more likely to...

Ready for Complex Open Enrollment Questions? AI Agents Can Help
AI agents are increasingly handling complex, personalized open‑enrollment questions, a shift highlighted by Cascade AI’s recent findings. The platform reports that open enrollment accounts for roughly 40% of labor costs, and one‑third of employee inquiries involve cost, coverage, or plan...

The Hidden Cost of Healthcare Data Breaches
Health‑insurance data breaches have exposed over 400 million identities since 2021, yet plan sponsors, TPAs and carriers provide no post‑breach fraud protection. HIPAA settlements can reach $25,000 per stolen identity, while remediation averages more than $13,000 per individual, creating a lucrative...

Looking Good: HSA, FSA Cover Rx Meta AI Glasses Through Truemed
Truemed has added Meta’s prescription‑compatible AI glasses to its HSA/FSA marketplace, joining popular wearables like Garmin watches and Oura rings. The partnership lets employees purchase Ray‑Ban and Oakley AI glasses using pre‑tax funds directly from the manufacturers’ sites. Integrated features...

This Resource Empowers Benefit Leaders to Support Caregivers
NEBGH launched a free microsite offering resources for benefit leaders to support employee caregivers. The platform compiles best‑practice guides, free external services, and benchmarking tools, drawing on input from senior benefit executives representing over nine million U.S. workers. It also...