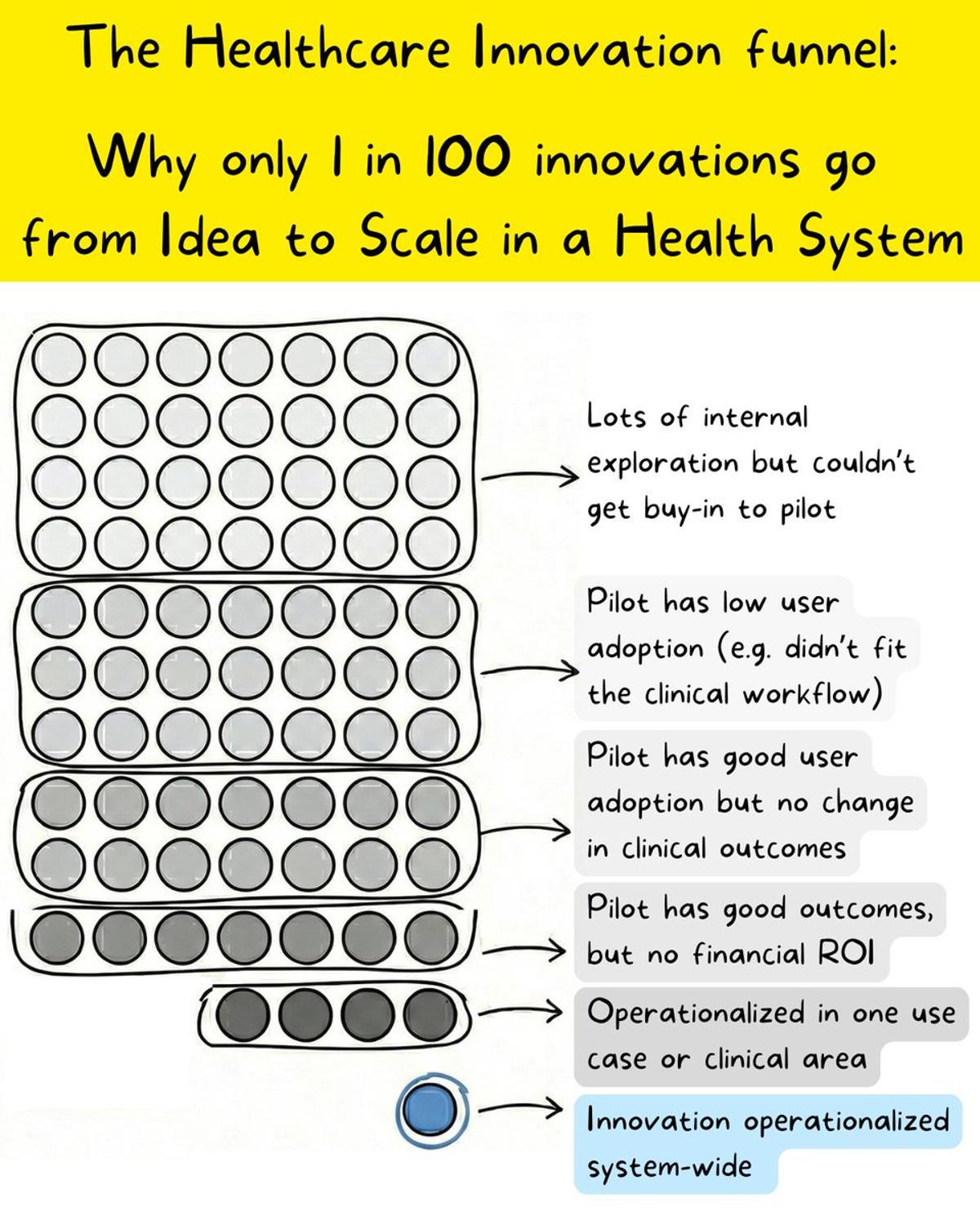
Most Health System Innovations Die Before Scaling
Many accuse health systems of not being willing to innovate. The truth? Lots of innovation is being explored all the time - you just don’t hear about them because most never make it to system-wide scale. For every 100 ideas that get explored within a health system: → 40 undergo lots of internal exploration but don’t achieve necessary buy-in to pilot. Maybe you have a clinical champion but lack buy-in from IT and leadership. Maybe you have top-down enthusiasm but no clinical champion. Lots of reasons ideas die here. → 30 pilots get launched but die off quick because of low user adoption. Maybe you couldn’t get it to fit the clinical workflow. Maybe there are too many competing priorities. Maybe the time to value is just too long. → 15 pilots have good user adoption but KPIs don’t improve. You figured out a way to successfully implement the innovation, but it doesn’t actually show a measurable improvement in clinical outcomes. It’s hard to create something that actually makes a difference on outcomes. → 10 pilots demonstrate improved clinical outcomes, but don’t translate to financial ROI from solving a real business problem - leading to no funding. There are lots of vitamins in healthcare, but only real painkillers tend to get sustainable funding. → 4 pilots demonstrate enough value and ROI to be operationally funded and sustained, BUT can’t grow beyond the initial use case or clinical area. It’s a niche innovation that only has executive sponsorship for a narrow area, but fails to reach escape velocity to justify system-wide transformation. → 1 innovation becomes operationally sustained enterprise-wide, leading to broad transformation across the health system. This is the innovation that the public catches wind of. Note that this isn’t specific to Health Tech - this is often the case for all types of innovation, including new models of care, clinical workflow innovations, AI models, etc. There is far more healthcare innovation being considered, tested and evaluated on an on-going basis than folks realize. It’s just honestly very difficult to earn the right to go from idea to pilot to local success to system-wide success. P.S. Please don’t hate me for there not being exactly 100 circles in the image. I just couldn’t convince the AI it to make the grid the way I wanted it to 😂

Stories, Not Data, Drive Health Tech Adoption
We want Health Tech to be evidence-based, but the truth is that adoption is ultimately driven by stories - NOT data. Here’s what I’ve seen play out over the past 13+ years over and over again: → Health system execs will choose...

AI Scribes Should Aid Notes, Not Replace Trainee Assessments
Should residents and med students get access to AI scribes? Or does it risk critically de-skilling them? My 7 thoughts: 1/ Students are increasingly using scribes in all aspects of their life. I’m not in school anymore but I suspect many...

Executive Passion Drives Successful Digital Health Journeys
Since 2020, health systems have diverged in Digital Health strategies for patient journeys (e.g. pre/postsurgery engagement). Two main camps: Camp 1: “We will deliver the best digital experience for patients that delivers the highest patient adoption, engagement and outcomes - we’re...
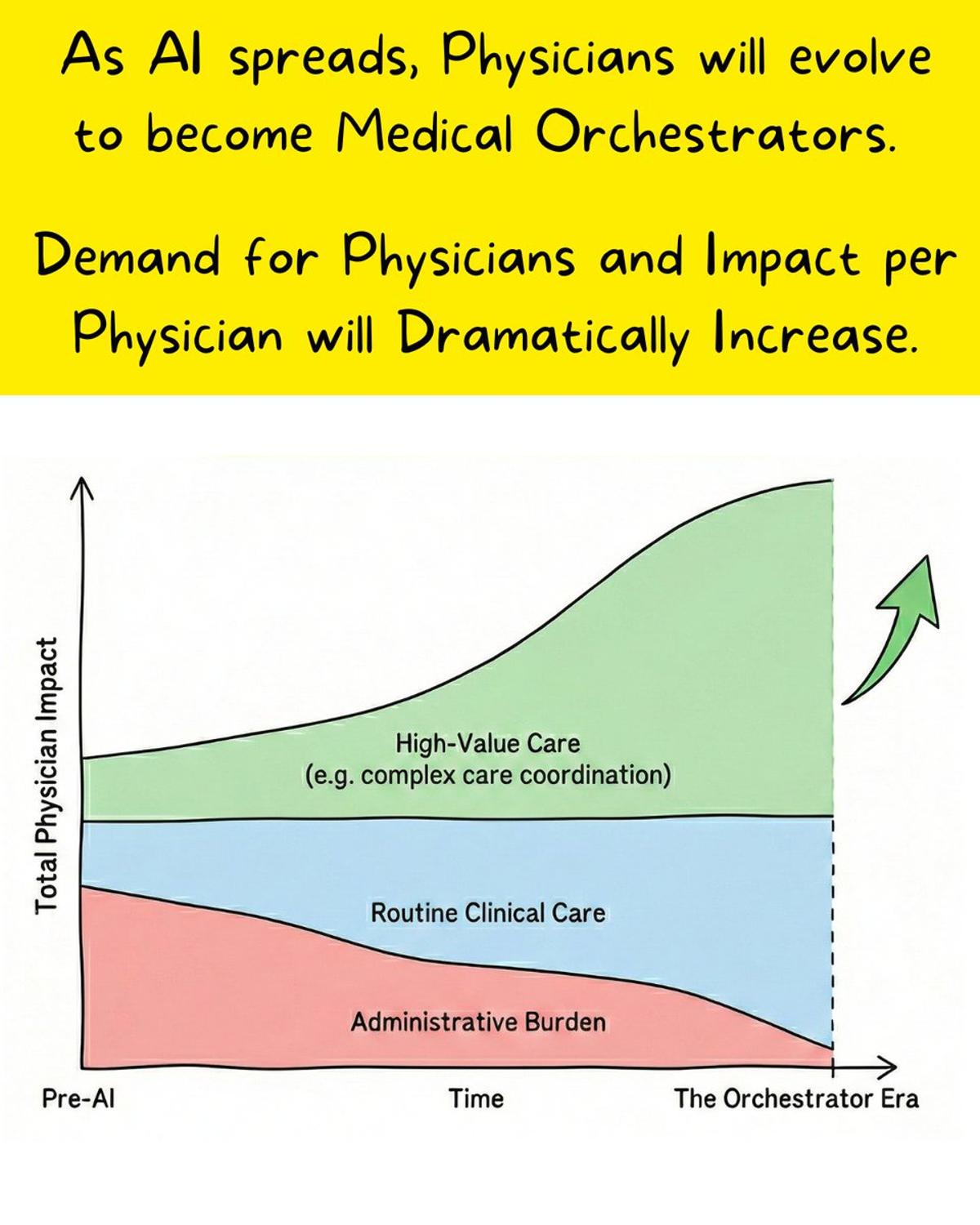
Physicians Evolve Into AI‑Guided Medical Orchestrators
Think AI will reduce demand for doctors? Consider this: Claude writes 100% of its own code, yet Anthropic's engineering team is exploding. We aren't looking at the end of the physicians, but the birth of Medical Orchestrators. When asked why Anthropic...

AI Docs Tools Expand Into Health System Enterprise
Those “direct-to-physician” CDS AI tools like OpenEvidence and DoximityGPT? They're now going after health systems too. My 5 thoughts on how this will all play out: First, the gist of what was announced: → Sutter Health will integrate OpenEvidence with Epic, allowing...